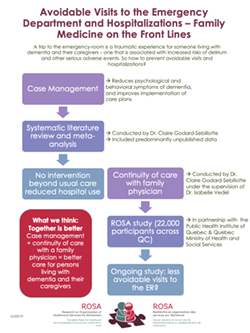
Assessing care models and policies implemented in primary health care for persons with neurocognitive disorders
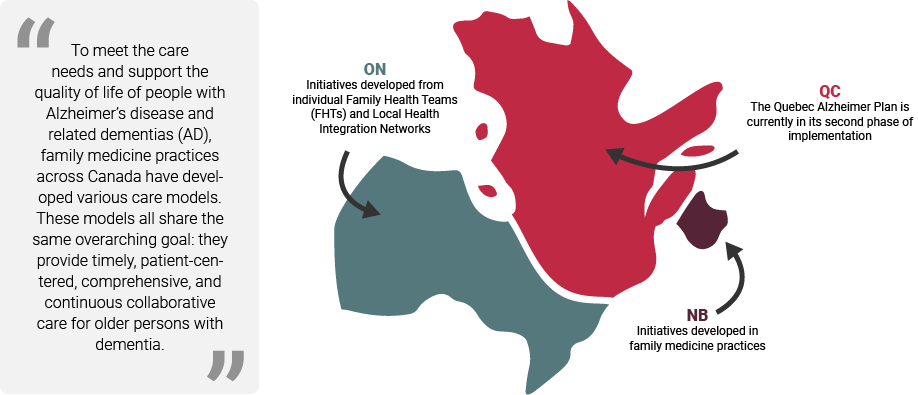
To see how we evaluated these models and initiatives, see our research objectives and methods
Preliminary results, news and program updates
Results:
Preliminary results in Quebec suggest that the Alzheimer Plan has had a beneficial impact on the quality of primary care for persons living with dementia and their caregivers. These results could be explained by the positive attitudes, practices, knowledge and competencies to detect, diagnose, treat and follow-up persons living with dementia in Family Medicine Groups.
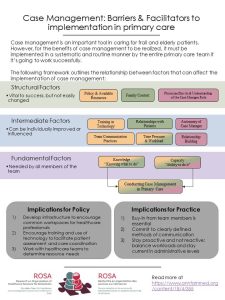
Finally, preliminary analyses suggest that the following elements must be present for the successful implementation of best practices: training and mentoring to clinicians; clinical tools; accompaniment by change managers; and identification of champions, case management mostly in the form of a dyad: physician-and-nurse. We have also been able to identify innovative practices that need to be scaled-up during phase 2.
Featured results:


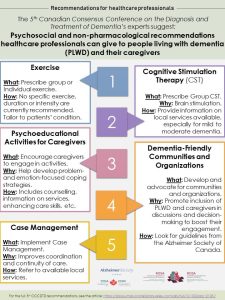
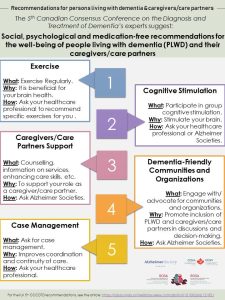
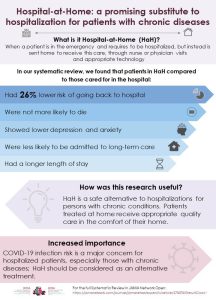
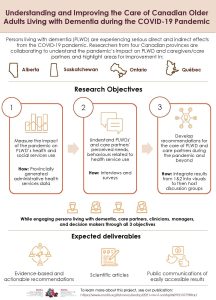
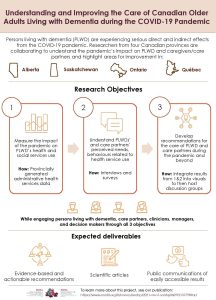
Publication list and media
Publications
Media
Co-Principal Investigators
The following page is authored by members of Team 19 of the Canadian Consortium on Neurodegeneration in Aging. Any questions regarding the content can be directed to: rosa-admin.fammed@Mcgill.ca